For us or against us? - The immune system as a cause of disease
FOR US OR AGAINST US? - THE IMMUNE SYSTEM AS A CAUSE OF DISEASE
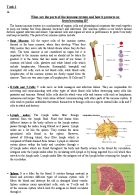
The immune system is equipped with a network of cells and tissues which enables the body to create a defence mechanism against invading organisms. It has evolved as a system poised to initiate and maintain protective responses against any harmful foreign element the body may encounter.9The cells in the immune system have the ability to distinguish between self or invader cells, and they try to get rid of invaders. However this system is not without flaws, autoimmune diseases are the result of specific immune responses directed against structures of the self .This happens as a result of the activation of B or T lymphocytes reacting against antigens of the body's own tissues. Myasthenia gravis is an example of a chronic autoimmune disease which affects the neuromuscular junction. Since muscle contraction depends on effective neuromuscular transmission between the nerves and muscles any interruption may lead to partial or complete paralysis. Weakness increases during periods of activity and improves after periods of rest. Certain muscles such as those that control eye and eyelid movement, facial expression, chewing, talking and swallowing are often involved in this disorder. The disease affects individuals of any age but the peak prevalence is amongst women in their twenties and men in their fifties and sixties.3
FIGURE 1
The immune system is composed of many cells; of these the white blood cells form the backbone. The white blood cells can be classified into five basic groups based on their functions. These are the basophils, eosinophils, macrophages and lymphocytes, the lymphocytes are further divided into B cells and T cells.
Table with cells of the immune system and their function
Cell Type
Functions
Macrophages
A macrophage is the first cell to recognize and engulf foreign substances (antigens). Macrophages break down these substances and present the smaller proteins to the T lymphocytes. Macrophages also produce substances called cytokines that help to regulate the activity of lymphocytes.
T cells( lymphocyte)
Types:
a) helper
b) killer
c) suppressor
a) Alert B cells to produce antibodies and stimulate macrophages as well as other lymphocytes.
b) attack and destroy diseased or infected cells
c) Slow down and stop the immune response of B and T cells.
B cells (lymphocyte)
Types:
a)plasma
b) memory
a) Responsible for creating of antibodies specific for an antigen.
b)these cells live for months or years and remain alert to detect any future attacks
Neutrophils
These are the first line of defense and perform phagocytosis. Their granules contain agents for killing microbes. Migrate from blood top sites of infection and inflammation.
Basophils
These release histamine, prostaglandis, etc, that promotes inflammation and increases mucous production. Involved in allergic reactions.
Eosinophils
They are capable of pagocytosis but primarily they release their contents into the surrounding environment to kill microbes extracellularly.
In an autoimmune response the helper T cells recognises cells of the body as foreign and mark them for destruction. We are usually free from this by a process called differentiation in the thymus whereby T cells with receptors for self-peptides are killed. This stage occurs in foetal development before birth. Each cell in the body is ...
This is a preview of the whole essay
Basophils
These release histamine, prostaglandis, etc, that promotes inflammation and increases mucous production. Involved in allergic reactions.
Eosinophils
They are capable of pagocytosis but primarily they release their contents into the surrounding environment to kill microbes extracellularly.
In an autoimmune response the helper T cells recognises cells of the body as foreign and mark them for destruction. We are usually free from this by a process called differentiation in the thymus whereby T cells with receptors for self-peptides are killed. This stage occurs in foetal development before birth. Each cell in the body is built with identification tags called MHC markers. In the thymus T cells under training interact with MHC molecules expressed on epithelial cells in the thymic cortex. As a result T cells become educated to MHC molecules expressed by the cortical epithelial cells. Hence for the rest of the life of the T cell it will only respond to antigens which are bound to the type of MHC molecules encountered in the thymus. During T cell selection within the thymus, MHC molecules presenting predominantly self antigens are present to achieve this result.
As the T cells interact with thymic epithelial cells in the thymus, the T cells with high affinity for self antigens are deleted. However some T cells with receptors specific for self antigens but with low affinity may escape.
FIGURE 2
Picture describing the neuromuscular junction
The voluntary muscles of the body are controlled by nerve impulses that arise in the brain. Nerve impulses travel down the nerves to the place where it meets the muscle fibres. The nerve fibres are not in direct contact with the muscle fibres the gap between them is known as the synaptic cleft. On one side of the synaptic cleft is the presynaptic membrane, on the other side the post synaptic membrane which is the surface membrane of the next neurone. Acetylcholine is a chemical messenger which is secreted at the ends of certain fibres; it transmits messages in the form of excitatory signals across the junction.
FIGURE 3
The neuromuscular junction sending a signal
When a neurone is not sending a signal, its inside is negative relative to the outside .This is due to the imbalance of sodium and potassium ions. The action potential is an explosion of electrical activity that is created by a depolarising current. When an action potential reaches the presynaptic membrane of the neurone, it causes calcium ions to diffuse in. The calcium ions cause vesicles containing acetylcholine to fuse with the presynaptic membrane releasing its contents into the synaptic cleft. The acetylcholine then diffuses across the cleft and binds to specific recognition site of receptors in the postsynaptic membrane. This results in opening of receptor operated ion channels, allowing pulses of inward ionic current (mainly Na+) to flow; this results in depolarisation.
If enough depolarisations are produced frequently enough, a muscle action potential and contraction results. In muscle a single impulse usually causes enough depolarization to reach threshold. The muscle action potential causes release of (Ca2+) from the sarcoplasmic reticulum of the muscle and this triggers muscle contraction .Acetylcholine diffuses away from its receptor site, the ion channel then closes.
The acetylcholine is then broken down by acetyl cholinesterase into inactive choline and acetate; this prevents unnecessary attachment to receptors and unwanted depolarisations. The resting potential of the fibre is then restored by an outflow of potassium ions.
FIGURE 4
Picture showing what happens at myasthenic junctions
The immune cells responsible for the autoimmune reaction in myasthenia gravis are the B cells and the T cells. For reasons which are still not understood the immune system attacks the nerve-muscle communication point in myasthenia gravis. The B cells produce antibodies against acetylcholine receptors on muscle fibres (described above). Although the production of acetylcholine-receptor antibodies is attributed to B cells, there is evidence that T cells have a key role to play in the autoimmune response of myasthenia gravis. About 80% to 90% of myasthenia gravis patients have serum antibodies of acetylcholine receptors that can be determined by a standard assay.
The acetylcholine receptor antibodies mentioned above can either block or cause damage to a receptor. It prevents the acetylcholine from attaching to its receptor hence the stimulus for a muscle contraction is reduced. The binding of antibodies to the receptor leads to the neuromuscular junction of myasthenia gravis patients having a decreased number of acetylcholine receptors.
FIGURE 5
Picture comparing the features between normal and myasthenic junctions
The following features are also associated to myasthenia gravis wider synaptic cleft and simplified folds of the postsynaptic membranes.Both wider and simplified synaptic cleft interact to reduce communication between acetylcholine and its receptors. At myasthenic junctions ,the decreased number of acetylcholine receptors results in end-plate potentials of diminished amplitude which fails to trigger action potentials; as the action potential follows the 'the all or none' principle. All-or-none means that there are not different size action potentials. When transmission fails at many junctions, the power of the whole muscle is reduced; this is manifested clinically as weakness.
Currently it is not certain how the immune response originated but one of the key theories is that the autoimmune process is initiated in the thymus. According to this theory a malfunction of the thymus gland may be involved. In addition to lymphocytes myasthenic thymus contain muscle-like cells (myoid) cells that bear surface acetylcholine receptors. Due to their location within the thymus surrounded by T cells and antigen presenting cells. The acetylcholine receptor bearing myoid cells may be susceptible to immune attack. Any alteration of the myoid cells or lymphocytes may lead to interference with tolerance and lead to an autoimmune response.
In most sufferers of myasthenia gravis the thymus gland is abnormal. Similarly 75% of myasthenia gravis patients have thymic abnormalities of these 85% have hyperplasia and 15% have thymomas. Several studies have shown that removal of the thymus increases the well being of the patients. Contradictory research on the other hand suggests that the thymus only builds up the immune system before puberty and has no effect thereafter.
Likewise other theories have also tried to explain how the immune system causes the disease using models other than the above mentioned. It is believed that during foetal development, the T cells with self peptides but with low affinity that escaped deletion remain dormant and may express themselves later on in life. This however may manifest itself as an autoimmune disease an example of which is myasthenia gravis. Another explanation is that in molecular mimicry the immune system may mistake portions of the acetylcholine receptor for portions of an invading virus; this is because some pathogens have similar structure to that of the host tissues. No candidate virus has yet been identified; this plays an important role in the immune response to infection in autoimmune diseases. Hence an infection may trigger the occurrence of the disease in some cases. Recent research has also shown that genes controlling other parts of the immune system, called MHC genes, appear to influence how susceptible a person is to developing autoimmune disease. However this like all other explanations of the disease is not a proven fact.
In short the immune system works for us but it could also turn against us. The exact reason why it turns against us is not known. However recent research proposes that the thymus gland is the most logical cause. The future looks very bright for sufferers of the disease because what used to be a grave muscle disease is no longer so. With recent research and technology mortality rate is essentially zero, this is due to optimal care and the different methods of treatments currently available. Despite these impressive advances, it is still not known the origin and the factors that contribute to this chronic disease.
References
. Mary J, Richard F, Dennis T. Advanced sciences Biology1. Cambridge: Cambridge university press; 2000. P.219-227.
2. Purves et al .The science of biology. 4th Ed. London : Sinauer Associates ;1998.p.9-16
3. Alan J. Neuromuscular function and disorders.1st ed. London: Butterworth and co publishers; 1977.p. 16-35.
4. Shepherd G. Neurobiology. 3rd Ed. New York: oxford university press;1994.p. 23-47
5. Angela V, Jackie P, David H. Myasthenia Gravis. The lancet 2001; vol 357:2122-8.
6. Eli B, Richard C, Geoffrey S. Immunology. 4th ed.chicester: Wiley publications; 2000. p. 135-9
7. Todd, Ian. Cells of the immune system. Nature encyclopaedia of life sciences. London: nature publishing group; 1999.www.els.net.(accessed October,2004)
8. Hale W, Saunders V, Margham J. Biology dictionary. 3rd Ed. Glasgow: Harper Collins publishers; 2003.
9. Sanders, Donald B. Myasthenia gravis In: Nature Encyclopedia of life sciences. London: nature publishing group; 2000.
10. Drachman D B, Adams R. Functional activities of acetylcholine receptors and the
Clinical severity of myasthenia gravis .New England Journal of Medicine 1982; vol
307: p 769-775
1. Groux H, O'Gara A, Bigler M. T cell subset inhibits antigen- specific T cell responses
.Nature 1971; vol 389; p737-742
2. Noel R, Ian R. the autoimmune diseases.3rd ed. London: Academic press; 1998.
p. 647-51.
3. Owen M, Lamb J. in: Male D editor. Immune recognition. 1st ed.Oxford: IRL Press
Limited; 1988.p.1-14
4. Drachman D.B: Myasthenia gravis. New England journal of Medicine 1994; vol.330
P.1797-1810.
15. Lahita G, Nicholas C, westley H. Text book of autoimmune disases.Philadelphia:
Maple press; 2000.p.640-5
16. Pauzzi M. Myasthenia gravis- A summary.2000. www.myasthenia.org (accessed
October, 2004)
17. FIGURE 1: William B.The immune system.1998. www.indexed visuals.
Com
18. FIGURE 2: Todd, Ian. The neuromuscular junction.2001. www.els.com
(Accessed October, 2004)
19. FIGURE 3: Vincent V, Jacie P, David H. Myasthenia gravis. The lancet 2001;
Vol 357:2122-8.
20. FIGURE 4: Barett EF.myasthenic junction.2002. www.patient.co.uk/myasthenia
Gravis. (Accessed October, 2004)
21. FIGURE 5: Drachman D.B: Myasthenia gravis. New England journal of Medicine
1994; 330; 1797-1810.
22.
MARILYN A.A. BOAKYE AGYEMAN
SPECIAL STUDIES ESSAY (FOUNDATION YEAR)