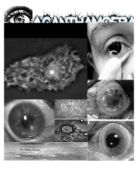
Acanthamoeba is found worldwide. Lakes, rivers, streams, swimming pools, hot tubs, air conditioning systems, soil, sewage systems, and even tap water are among the places where this parasite can be found. Conditions such as hypersomolarity, glucose starvation, desiccation, or extreme PH levels and temperatures up to 42 degrees Celsius, are unfavorable; the parasite turns into a cyst to evade these conditions.
Acanthamoeba can be spread into the eyes through contact lens use, cuts, skin wounds, or even by being inhaled into the lungs. Most people will be exposed to the parasite during their lifetimes; however, very few become sick from the exposure. The most common way Acanthamoeba makes its way into the eye is via water, usually pools and lakes, from recreational activities, or during the routine use of contact lenses. In the United States, one or two out of every one million users of contact lenses will contract the disease.
The clinical symptoms and signs of acanthamoeba keratitis can be easily confused with other corneal infections. During the onset of the disease process, patients may experience blurred vision, photophobia, tearing, involuntary tight closure of the eyelids, and foreign body sensation. Other symptoms include severe ocular pain, inflammation, swelling, or even vision loss. The symptoms tend to increase and decrease, depending on the rapidity of the onset as well as the severity of the chronic keratitis and the anterior chamber inflammatory reaction. Additional clinical signs may include corneal microcysts, bullous keratopathy, corneal ulcers, eye redness, and conjunctival discharge.
Diagnosis of acanthamoeba keratitis is very difficult. The first step is to suspect it, especially in patients who wear contact lenses with corneal involvement who are experiencing pain resembling herpes simplex keratitis. If the patient has a history of ocular exposure to soil, contaminated water or a history of minor ocular trauma, this increases suspicion significantly. The ophthalmologist will then proceed to five common ocular examinations: visual acuity, refractory test, tear test, slit lamp biomicroscopy examination, and a pupillary reflex response test. Another option is to obtain a laboratory diagnosis. This involves scraping the involved epithelium and stroma of the cornea with a sharpened kimura spatula, and then culturing the tissue for organisms. If the patient is a contact lens wearer, then the lenses, lens case, and solutions are cultured as well.
In the United States, cases of acanthamoeba keratitis increased substantially during the 1980’s with the introduction of disposable soft contact lenses. Modern evidence shows that the rate has dropped afterwards, especially with the introduction of multipurpose cleaning solutions. The estimated rate of Acanthamoeba keratitis is 1 per 250,000 people in the United States. Around 25 million people wear contact lenses in the U.S. But very few actually contract this parasite, and fewer lose their sight as a result. The mortality of the disease is non-threatening, keratitis is a local infection that does not lead to systemic infection or death but may be complicated by cataracts, hypopyon, increased intraocular pressure, and can even threaten eyesight.
Killing this parasite is extremely difficult because the Acanthamoeba is a “master of disguise”. Acanthamoeba has two separate forms: active- when it’s feeding and moving around, living off of its environment and inactive- when the environment becomes hostile, a cyst, where it’s very tough and protected, waiting for things to get better. Successful treatment of keratitis consists of early diagnosis and aggressive surgical and medical therapies. Medical treatment consists of topical antimicrobial agents, which can achieve high concentrations at the site of the infection. Because the acanthamoeba cyst may be highly resistant to therapy, a combination of agents is generally used. The topical antimicrobials are administered every hour immediately after corneal damage. The agents are then continued hourly for 3 days, at least nine times a day. The frequency is then reduced to every 3 hours. After two weeks, the response from the drugs is then observed. The normal total duration of therapy is a minimum of 3-4 weeks, while extreme cases can take 6-12 months. When a patient under goes surgical care, the dead or contaminated tissue is cut away from the abnormal epithelium to prevent further infection. In some serious cases, corneal transplants may be necessary.
To minimize the risk of catching Acanthamoeba, contact wearers, who are most at risk, can reduce the risk of infection by having regular eye examinations and keeping contact lenses and their cases clean. This includes washing hands with soap and water before handling lenses, cleaning lenses according to manufacturers’ guidelines, using fresh disinfecting solution each time lenses are cleaned and stored, rinsing storage cases with sterile solution (never tap water!) and leaving them open to dry, and replacing storage cases once every three months. Contact lenses should also be removed before any activity involving water, including showering, using a hot tub or swimming. People who don’t wear contact lenses can also get infected, especially if the cornea is scratched.
I chose this as my topic because my interests in parasites are large. You wouldn't normally suspect that such a common thing - contact lenses - could carry such a risk.
When I was looking around online this is one parasite that I found interest in and wanted to learn more about. Its interesting how such a small organism can do so much damage to our bodies, not to mention the fact that they are all around us!
Works Cited
-
Centers for Disease Control and Prevention. Parasites - Acanthamoeba. 10 March 2011. 24 January 2012 <http://www.cdc.gov/parasites/acanthamoeba/>.
-
Clinical Microbiology Reviews. Acanthamoeba spp. as Agents of Disease in Humans. 4 February 2006. 24 January 2012 <http://cmr.asm.org/content/16/2/273.full>.
-
Discovery Communications, LLC. Monsters Inside Me Acanthamoeba Keratitis. 22 July 2011. 24 January 2012 <http://animal.discovery.com/invertebrates/monsters-inside-me/acanthamoeba-keratitis/>.
-
RICHARD L. ABBOTT, MICHAEL ZEGANS and TROY R. ELANDER. Acanthamoeba Keratitis. 23 September 2010. 24 January 2012 <http://www.oculist.net/downaton502/prof/ebook/duanes/pages/v4/v4c018a.html>.
-
Safar, Elmeya H. "Involvement of the eye with Acanthamoeba." Journal of The Arab Society for Medical Researches 3 (2010): 191-198.
-
The Eye-Eating Parasite. Dir. MONSTERS INSIDE ME. Animal Planet. Discovery Communications. Discovery Communications, LLC, 2009.
**polymorphonuclear: Having a lobed nucleus. Used especially of neutrophilic white blood cells.