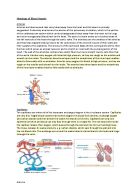
Unlike the arteries and veins, capillaries are very thin and fragile. The capillaries are actually only one epithelial cell thick. They are so thin that blood cells can only pass through them in single file. The exchange of oxygen and carbon dioxide takes place through the thin capillary wall. The red blood cells inside the capillary release their oxygen which passes through the wall and into the surrounding tissue. The tissue releases its waste products, like carbon dioxide, which passes through the wall and into the red blood cells.
Arteries and veins run parallel throughout the body with a web-like network of capillaries, embedded in tissue, connecting them. The arteries pass their oxygen-rich blood to the capillaries which allow the exchange of gases within the tissue. The capillaries then pass their waste-rich blood to the veins for transport back to the heart.
Capillaries are also involved in the body's release of excess heat. During exercise, for example, your body and blood temperature rises. To help release this excess heat, the blood delivers the heat to the capillaries which then rapidly release it to the tissue. The result is that your skin takes on a flushed, red appearance. If you hold your hand, for example, under hot water, your hand will quickly turn red for the same reason. Your arm, however, is not likely to change colour because it is not actually feeling an increase in temperature. (www.fi.edu)
- Explain the way in which blood circulates through the heart. Describe how the heartbeat is initiated and modified to meet all situations.
When someone listens to your heart with a stethoscope the sound is often described as lub-dub lub-dub. The first heart sound (lub) is caused by the acceleration and deceleration of blood and a vibration of the heart at the time of the closure of the tricuspid and mitral valves. The second heart sound (dub) is caused by the same acceleration and deceleration of blood and vibrations at the time of closure of the Pulmonic and aortic valves.
The heart beat is caused by impulses arising from two specialised groups of cells within the heart muscle. The Sino-Atrial (SA) node, situated in the wall of the right atrium initiates the beat, and the Atrioventricular (AV) node which is positioned between the ventricles and continues to distribute the wave of impulses. This pacemaker generates electrical impulses at a given rate, but emotional reactions and hormonal factors can affect its rate of discharge. This lets the heart rate respond to varying demands
There are several distinct stages which form a full heart beat. Cardiac Systole describes the period at which the heart contracts and cardiac diastole describes the period of relaxation, between beats. They can however be further divided into diastole and systole of the atria and ventricles. (www.teachpe.com)
The average heartbeat is 72 times per minute. In the course of one day it beats over 100,000 times. In one year the heart beats almost 38 million times, and by the time you are 70 years old, on average, it's made it to 2.5 billion beats.
The electrical impulse leaves the SA node (1) and travels to the right and left atria, causing them to contract together. This takes .04 seconds. There is now a natural delay to allow the atria to contract and the ventricles to fill up with blood. The electrical impulse has now traveled to the atrioventricular node (AV node) (2). The electrical impulse now goes to the Bundle of His (3), then it divides into the right and left bundle branches (4) where it rapidly spreads using Purkinje fibers (5) to the muscles of the right and left ventricle, causing them to contract at the same time.
Any of the electrical tissue in the heart has the ability to be a pacemaker. However, the SA node generates an electric impulse faster than the other tissue so it is normally in control. If the SA node should fail, the other parts of the electrical system can take over, although usually at a slower rate. (health.howstuffworks.com) although the pacemaker cells create the electrical impulse that causes the heart to beat, other nerves can change the rate at which the pacemaker cells fire and the how strongly the heart contracts. These nerves are part of the autonomic nervous system. The autonomic nervous system has two parts - The sympathetic nervous system and the parasympathetic nervous system. The sympathetic nerves increase the heart rate and increase the force of contraction. The parasympathetic nerves do the opposite. (health.howstuffworks.com)
Everyone's pulse (average heart rate per minute) changes as we age. The following is a table of the average pulse rates at different ages:
Our pulse rate increases or decreases in reaction to certain conditions, for instance the pulse rate will increase during exercise as we need more oxygen to circulate around our body to help the muscles and organs to work, the pulse rate will also decrease for example during times hypothermia the pulse will slow down and only pump blood to the to most important organs such as the lungs and the brain it will draw the blood away from the surface of the skin and is the reason we look blue when we are very cold. Our blood pressure is also controlled by the heart and this is regulated by the cardiac output (i.e. the strength of the contraction of the ventricles) and the diameter of the blood vessels. Increased blood flowing to the heart causes the muscle of the heart to stretch and the more it is stretched, the stronger it contracts increasing blood pressure.
If the arterioles that supply the tissues are constricted then the blood pressure will rise, as it is difficult for the heart to pump the blood. If the arterioles dilate then the blood pressure will fall. The diameter of these vessels is controlled by the cardiovascular centre of the brain.
The condition known as Arteriosclerosis (‘furring up’ of blood vessels) reduces blood flow and leads to high blood pressure. A blood clot forming at an arteriosclerotic site can prevent blood flow. If this is occurs in the coronary vessels supplying the heart then a heart attack results or if it is in vessels supplying the brain a stroke results. The lack of oxygen can result in permanent damage to the heart muscle or an area of the brain depending upon how long the vessel is blocked. (Class notes)
- Discuss the structure of the blood and relate this to the function. Explain the problem that can occur when transfusing blood.
Although blood looks like a red liquid, if some is left in a test tube it separates out into pale liquid called plasma and a solid layer of blood cells.
Major components of blood -made up of the following things:
Plasma - Blood cells are suspended in the plasma. Plasma makes up 55% of the blood. Made up mostly of water (90%) it carries a number of important things like:
-
Fibrinogen - plasma proteins made in the liver involved in blood clotting.
-
Gamma globulins - plasma proteins made in the liver involved in fighting infections (immunoglobulin’s = antibodies)
-
Albumin -plasma proteins that maintain the high osmotic potential of the plasma preventing loss of fluid from the bloodstream to the tissues.
-
Angiotensinogen - Involved in re-absorption of sodium and control of blood volume and blood pressure.
-
Nutrients - (glucose, fats and amino acids).
-
Gases - oxygen and carbon dioxide
-
Miscellaneous substances - various ions, hormones, and waste materials (e.g. urea and ammonia.) (www.cancerhelp.org.uk)
Cellular Layer
In order to investigate the different cells in the blood we need to produce a blood smear on a slide and examine it under the microscope. If we do this the following cells can be identified. (Class notes)
The blood is about 55% plasma and 45% cells. Plasma is mostly water with some proteins and other chemicals dissolved in it. There are three main types of cells in the blood
-
-
White Blood Cells
There are several different types of white cells in the blood in differing amounts. They all play a part in the immune response. This is the response of the body to infection, or anything else the body recognises as 'foreign'. These blood cells can be made very quickly and generally have a short life. Some only live for a few hours, others for days.
There isn't an exact 'normal' figure for blood counts. 'Normal' for a large man wouldn't be the same as for a small woman. But generally the normal white cell count is between about 4,000 and 11,000 per cubic millimeter of blood. If you have surgery or an infection, your white blood cell counts will go up within a day or two.
The most numerous of the white blood cells are the neutrophils. There are between 2,000 and 7,500 of these per cubic millimeter of blood. They are important for fighting infection. If you have chemotherapy, particularly in high doses, your neutrophil count usually drops quite quickly. (www.cancerhelp.org.uk)
the next most numerous are the lymphocytes. Any invading pathogen acts as an antigen which is something foreign to the body. Their antigens stimulate the lymphocytes and monocytes to produce specific antibodies against antigens. The antibody combines with the antigen to render it harmless. The antigen, antibody complex can now is destroyed by the phagocitic polymorph cell as describes previously. (Class notes)
A normal lymphocyte count is between 1,300 and 4,000 per cubic millimeter of blood.
Other white blood cells are present in smaller numbers in the circulating blood. There are between
- 40 and 400 eosinophils
- 0 and 100 basophils
- 200 and 800 monocytes
per cubic millimeter of blood. As we've said, the range quoted as normal for blood cell counts varies. These figures are taken from the Oxford Handbook of Clinical Medicine. (www.cancerhelp.org.uk)
Red Blood Cells:
These are by far the most numerous of the blood cells. They are sometimes referred to as BICONCAVE DISC SHAPED CELLS, they are basically a cell membrane packed full of the red pigment HAEMOGLOBIN. Their function is to carry oxygen around the body. The haemoglobin had the ability to easily pick up oxygen as the cells pass through the lungs and give up oxygen to the cells. (Class notes)
OXYGEN + HAEMOGLOBIN OXYHAEMOGLOBIN
When the haemoglobin is oxygenated it is bright red and when it looses its oxygen it is dark red this is what gives red blood cells its red colour. There are more than 4 or 5 million red blood cells in every cubic millimeter of blood. A red blood cell can live for up to 120 days.
Red blood cells are able to attach to oxygen to carry it within the circulation to the tissues. When they get to an area where the oxygen is needed, they give it up and pick up carbon dioxide which they carry back to the lungs. A shortage of red blood cells is called anemia. The role of the red blood cell in carrying oxygen explains why very anemic people usually feel breathless.
Platelets
Platelets are really bits of much bigger cells called megakaryocytes. A normal platelet count is between 150,000 and 440,000 per cubic millimeter of blood.
Platelets are very important in blood clotting. They clump together to form a plug if bleeding occurs. Then they release other chemicals that help the blood to clot and the blood vessel to be repaired. (www.cancerhelp.org.uk)
how and where blood cells are made
all the different types of blood cells develop from one type of cell called a 'blood stem cell'. In adults, blood stem cells are normally found in the red bone marrow inside the bones. Blood cells are made in the bone marrow in the skull, ribs, sternum (breast bone), spine and pelvis.
The stem cells divide and multiply to make the blood cells. These cells differentiate (develop and mature) as they grow into white cells, red cells or platelets. The diagram below shows how the various different types of cells can develop from a single blood stem cell. (www.cancerhelp.org.uk)
Blood Groups and Blood Transfusion
Group a Blood
Group a blood has antigens on the red blood cell and naturally occurring B antibodies in the plasma.
Group B Blood
This group has B antigens on the red blood cell and naturally occurring antibodies in the plasma.
Group AB Blood
This has A + B antigens on the red blood cells but neither A or B antibodies in the plasma.
Group O Blood
This has neither A or B antigens on the red blood cell but both A and B antibodies in the plasma.
The above blood groups are the most common blood groups; it does not matter which blood group you are until a transfusion is required, the following table shoes which blood groups can be transfused:
From the table it can be seen that O is the universal donor and AB is the universal recipient. (Class notes)
The ABO system also contains lots of little antibodies in the plasma, antibodies being the body's natural defence against foreign antigens.
This means giving someone blood from the wrong ABO group could be fatal.
The anti-antibodies in group B attack group cells and vice versa.
This is why group a blood must never be given to a group B person. (www.blood.co.uk)
Although very rarely occurring there are a few side effect and negative reactions to being given blood transfusions other than the ones occurring when the wrong blood group have been given and it is very rare for people to catch other disease from having a blood transfusion as the blood is screened before being passed on to others for transfusion:
Allergic Reaction
Some people have allergic reactions to the blood given during transfusions. This can happen even when the blood given is the right blood type.
Allergic reactions can be mild or severe. Symptoms can include:
- Anxiety
- Chest and/or back pain
- Trouble breathing
- Fever, chills, flushing, and clammy skin
- A high pulse or low blood pressure
- Nausea (feeling sick to the stomach)
A transfusion is stopped at the first signs of an allergic reaction. The health care team determines how mild or severe the reaction is, what treatments are needed, and if the transfusion can safely be restarted.
Viruses and Infectious Diseases
Some infectious agents, such as HIV, can survive in blood and infect the person receiving the blood transfusion. To keep blood safe, blood banks carefully screen donated blood.
There is a risk of catching a virus from a blood transfusion, but it's very low.
- HIV. Your risk of getting HIV from a blood transfusion is lower than your risk of getting killed by lightning. Only about 1 in 2 million donations may carry HIV and transmit HIV if given to a patient.
- Hepatitis B and C. The risk of having a donation that carries hepatitis B is about 1 in 205,000. The risk for hepatitis C is 1 in 2 million. If you receive blood during a transfusion that contains hepatitis, you will likely develop the virus.
-
Variant Creutzfeldt-Jakob disease (vCJD). Variant CJD is the human version of Mad Cow Disease. It's a very rare, yet fatal brain disorder. There is a possible risk of getting vCJD from a blood transfusion, although the risk is very low. Because of this, people who may have been exposed to vCJD aren't eligible blood donors. Fever
You may get a sudden fever during or within a day of your blood transfusion. This is usually your body's normal response to white blood cells in the donated blood. Over-the-counter fever medicine will usually treat the fever.
Some blood banks remove white blood cells from whole blood or different parts of the blood. This makes it less likely that you will have a reaction after the transfusion.
Iron Overload
Getting many blood transfusions can cause too much iron to build up in your blood (iron overload). People with a blood disorder like thalassemia, which requires multiple transfusions, are at risk of iron overload. Iron overload can damage your liver, heart, and other parts of your body.
If you have iron overload, you may need iron chelation therapy. For this therapy, medicine is given through an injection or as a pill to remove the extra iron from your body.
Lung Injury
Although it's unlikely, blood transfusions can damage your lungs, making it difficult to breathe. This usually occurs within about 6 hours of the procedure. Most patients recover. However, 5 to 25 percent of patients who develop lung injuries die from the injury. These people usually were very ill before the transfusion.
Doctors aren't completely sure why blood transfusions damage the lungs. Antibodies (proteins)—which are more likely to be found in the plasma of women who have been pregnant—may disrupt the normal way that lung cells work. Because of this risk, hospitals are starting to use men and women's plasma differently.
Acute Immune Haemolytic Reaction
Acute immune haemolytic reaction is very serious, but also very rare. It occurs if the blood type you get during a transfusion doesn't match or work with your blood type. Your body attacks the new red blood cells, which then produce substances that harm your kidneys.
The symptoms include chills, fever, and nausea, pain in the chest or back, and dark urine. The doctor will stop the transfusion at the first sign of this reaction.
Delayed Haemolytic Reaction
This is a much slower version of acute immune haemolytic reaction. Your body destroys red blood cells so slowly that the problem can go unnoticed until your red blood cell level is very low.
Both the acute and delayed haemolytic reactions are most common in patients who have had a previous transfusion.
Graft-Versus-Host Disease
Graft-versus-host disease (GVHD) is when white blood cells in the new blood attack your tissues. GVHD is usually fatal. People who have weakened immune systems are the most likely to get GVHD.
Symptoms start within a month of the blood transfusion. They include fever, rash, and diarrhoea. To protect against GVHD, patients with weakened immune systems should receive blood that has been treated so the white blood cells can't cause GVHD. (www.nhlbi.nih.gov)
REFERENCES and BIBLIOGRAPHY:
http://mcb.berkeley.edu/courses/mcb135e/arteries.html
http://www.ivy-rose.co.uk/Topics/Blood_Vessels.htm
Lee, M. (2009). ‘Biology 2: The Human Circulatory System (Blood System) Class Notes’ Bishop Auckland College 17/03/09
Lee, M. (2009). ‘Biology 2: The Human Circulatory System (Blood System) Hand Out Bishop Auckland College 17/03/09
Lee, M. (2009). ‘Biology 2: The Structure and Functions of the Blood Class Notes.’ Bishop Auckland College 24/03/09
Lee, M. (2009). ‘Biology 2: The Nervous and Hormonal Control of the Blood System Handout.’ Bishop Auckland College 24/03/09
Lee, M. (2009). ‘Biology 2: Blood Vessels Hand out.’ Bishop Auckland College 24/03/09
http://www.fi.edu/learn/heart/vessels/veins.html
http://www.teachpe.com/anatomy/circulatory_system.php
http://www.americanheart.org/presenter.jhtml?identifier=4642
http://health.howstuffworks.com/heart1.htm
http://www.nhlbi.nih.gov/health/dci/Diseases/bt/bt_risk.html
http://www.blood.co.uk/pages/e13basic.html
Waugh, A & Grant, A (2001). ‘Anatomy and Physiology in Health and Illness Ninth Edition’. Churchill Livingston, UK.
Vander, A. Sherman, J. & Luciano, D (1998). ‘Human Physiology The Mechanisms of Body Function Seventh Edition’. WCB/McGraw-Hill, USA.