Uric acid is a much larger molecule than urea. It is a purine, similar in structure to adenine and guanine. Energy from metabolism is required in the formation of uric acid, but once formed it is virtually insoluble and therefore non-toxic to the organism. Uric acid is produced as a colloidal suspension. Further water absorption leads to crystals of urates being formed. These are discharged as thick paste or as solid pellets. Uric excretion (uricotelic excretion) occurs in organisms, which develop in an enclosed egg (where water is severely limited), or which normally experience a very dry terrestrial environment as adult organisms.
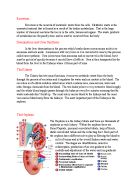
The excretory organ of mammals is the kidney. A pair of kidneys occurs in the dorsal wall of the body cavity, the coelom, with a supply of blood from the dorsal aorta via renal arteries, and drained by renal veins. The functional unit of the kidney is a tiny elongated tubule, the renal tubule or nephron. A kidney consists of a large number of nephrons, which eventually empty into a single duct, the ureter, running to the exterior of the body. At one end of the nephron, blood supply and tubule are in close association in a structure called the Malpighian body. This consists of a cup-shaped chamber, the renal capsule, which encloses a knot of capillaries known as the glomerulus. In the glomerulus blood pressure forces part of the plasma out of the thin capillary walls. The capillary walls prevent the blood cells and protein molecules from passing through, so the filtered fluid is like tissue fluid. The filtrate passes from the renal capsule down the remainder of the tubule, and on this journey useful metabolites are selectively reabsorbed. Additional waste substances may also be actively secreted into the ultra filtrate from the cells of the wall of the tubule. These processes form the excreted liquid, urine.
The composition of body fluids is influenced more by output by the kidneys than by intake via the gut, and therefore the kidneys are important guardians of the internal environment. By means of the regulated production of urine from the blood the nephrons carry out the dual process of excretion and osmoregulation. Excretion occurs by lowering of the blood levels of urea and of any other toxic compounds present.
The daily output of urine contains about 50g solid matter, the chief components being urea (30g) and sodium chloride (15g). Also present is the surplus of other metabolites and inorganic ions from catabolism. The pH of the blood is kept constant at 7.4; that of urine varies according to whether excess of hydrogen or of hydroxide ions has been absorbed in the food.
The operation of the nephron involves several distinct mechanisms. They include:
- Ultrafiltration - high blood pressure in the glomerulus forces water and other small molecules in the plasma through the walls of the capillaries and of the renal capsule into the tubule lumen, a process known as ultrafiltration.
- Selective re-absorption- those components of the filtrate in the nephron which are useful to the body are re-absorbed in the blood system by active transport across the cells of the tubule wall. These re-absorbed substances include amino acids and glucose, as well as other compounds, to maintain the water and salt composition of the body fluids.
- Secretion- other substances, not required by the body, are added to the filtrate from the body by active transport from the cells of the tubule wall.
- Differential permeability- parts of the walls of the tubule are impermeable to water, ions or urea; these substances thus cannot diffuse or be transported back into the blood in those regions. Hormones control the permeability of the walls of the collecting duct and the distal convoluted tubule.
- Urine storage- the urine passes to the bladder via long tubes, the ureters, and is stored there. The bladder is a dispensable sac with a wall of smooth muscle lined by a special type of epithelium, known as a transitional epithelium. The bladder can hold 400-500 ml of urine. Once 200 ml or so has been collected stretch receptors are stimulated, and this stimulation initiates the desire to discharge the urine. The urine passes to the exterior through the urethra. Spincter muscles close the exit from the bladder.
Urine formation is carried out in the following way:
- Ultrafiltration in the renal capsule - ultrafiltration occurs from the capillaries of the glomerulus into the lumen of the renal capsule, due to the pressure of blood in the kidney and the sieve-like quality of the walls of the glomerular capillaries and the renal capsule. the sieve action permits many smaller sized molecules to pass through, but retains in the blood almost all the blood proteins (and blood cells)
The capillaries of the glomerulus are more permeable than capillaries elsewhere in the body. This permeability is due to the presence of numerous pores or fenestrations (0.1 nano metre in diameter) between the endothelium cells that make up the capillary wall. These cells are attached to the basement membrane, through which the filtrate next passes. This basement membrane is a continuous layer. As a consequence, whilst much of the plasma passes through, all blood proteins and cells are retained within the arterioles. The final part of the sieve mechanism consists of the walls of the renal capsule. The cells of these walls, instead of forming a continuous sheet, are organised into an irregular-supporting network. The filtrate, having passed between the endothelium cells ad through the basement membrane, now passes into the capsule via large, slit-like pores between these processes.
The blood pressure in the glomerulus is high because the diameter of the efferent arteriole is much less than that of the afferent arteriole. A hydrostatic pressure is generated, which forces molecules of r.m.m below about 68 000 into the renal capsule. These molecules include glucose, amino acids, vitamins, some hormones, urea, other simple nitrogenous compounds, ions and small proteins, and also some of the water. Retained in the blood are red and white cells, platelets, most plasma proteins and the rest of the water.
A volume of blood equivalent to that in the whole body passes through the kidneys every four or five minutes. This means that every minute the kidney's process 1200-ml of blood. Of this, 650 ml is plasma. About 125 ml of this plasma (one-fifth of the volume) is filtered out into the capsules. In all, about 180 litres of the filtrate is formed each day, but obviously far less is lost from the body as urine. As the filtrate flows along the remainder of the tubule its composition is changed, and much is re-absorbed. The quantity of urine finally formed is 1-1.5 litres per day, or about 1 ml per minute.
- Reabsorbtion in the proximal convoluted tubule - active reabsorbtion of the glomerular filtrate occurs in the proximal convoluted tubule, and a large part of the filtrate is re-absorbed into the capillary network here. Example glucose, amino acids. Sodium ions are pumped from the filtrate into the proximal convoluted tubule cells, and then actively transported into the fluid of the inter cellular spaces. This movement of dissolved substances from filtrate into the blood capillary network brings about the osmotic movement of water in the same direction. In this way about 70% of the water in the filtrate is reabsorbed from the proximal convoluted tubule into the blood of the capillary.
About 50% of the urea in the filtrate diffuse back into the blood here, because of the concentration differences generated by the water reabsorbtion between the filtrate, the proximal convoluted tubule cells and the blood.
In the proximal convoluted tubule, the cells actively excrete poisonous substances from the blood into the filtrate, along with some nitrogen containing substances such as creatinine. Any blood proteins forced into the filtrate by extra high blood pressure in the glomerulus are taken out of the filtrate here by pinocytosis at the base of the microvilli. As a result of these processes a much reduced volume of filtrate, isotonic with the body fluids, passes into the loop of Henle
- The Loop of Henle - here water conservation takes place.
A counter current multiplier occurs in the Loop of Henle. The effect of the counter current exchange mechanism of the loop of Henle is to build up the concentration of ions across the medulla. An increasing concentration of ions in the medulla facilitates the later withdrawal of water, mostly from the collecting ducts.
The other counter current mechanism in the medulla of the kidney occurs in the vasa recta, the blood vessels serving this region of the kidney. They have dual role to deliver nutrients to the cells of the medulla, and to carry water reabsorbed from the filtrate.
- Regulation in the distal convoluted tubule
The role of the cells of the wall of the distal convoluted tubule is the fine control of blood composition. The cell contents include mitochondria for energy supply.
The pH is maintained at a constant value of 7.4. Abrupt change in blood pH is prevented by the presence in the plasma of proteins, while hydrogencarbonate and phosphate ions act together as buffers. The cells of the distal tubule also regulate the plasma concentrations of ions such as sodium, chloride and calcium. Whenever necessary these ions are removed from the urine into the blood by active transport across the tubule wall.
- Water reabsorbtion in the collecting duct - the permeability to water of the walls of the collecting duct is controlled by a hormone know as antidiuretic hormone (ADH), secreted by the pituatry gland. When the walls are made permeable water is reabsorbed from the urine in the collecting duct by osmosis, as a result of the high salt concentration in the medulla, through which the collecting duct runs. When the walls are impermeable, however, no water is lost from the urine as it travels down the collecting duct…. Control by ADH secretion leads to the production of hypotonic or hypertonic urine, according to the body's varying demand for water.
Urine formed by the kidneys is temporarily stored in the bladder. Emptying of the bladder, known as micturition, normally occurs well before the limit capacity is reached. Micturition takes place by contraction of the bladder wall and relaxation of the spinchter muscles at the neck of the bladder. The bladder wall consists of smooth muscle, which is under the control of the autonomic nervous system. Micturition is a reflex response to stretching of the walls. The reflex becomes suppressed by voluntary nervous action.